Published April 29, 2026
By Dr. Richard Nguyen, Board-Certified General Surgeon
Making the decision to pursue bariatric surgery is a profound step toward reclaiming your health, mobility, and quality of life. For many patients in San Jose, Los Gatos, and the greater South Bay area, the journey begins with a critical question: which procedure is the right fit? The two most common and effective weight loss surgeries performed today are the gastric sleeve (sleeve gastrectomy) and the gastric bypass (Roux-en-Y). Both procedures offer life-changing results, but they work in different ways and are suited to different patient profiles.
As a fellowship-trained surgeon at Vanderbilt who now specializes in bariatric surgery and minimally invasive surgery here in the Bay Area, I spend a significant amount of time helping patients navigate this exact decision. My goal is to provide you with a comprehensive, patient-friendly comparison of the gastric sleeve vs gastric bypass, covering their mechanisms, expected weight loss, recovery processes, risks, nutritional considerations, and insurance implications. By understanding the nuances of each procedure, you can make an informed choice that aligns with your long-term health goals.
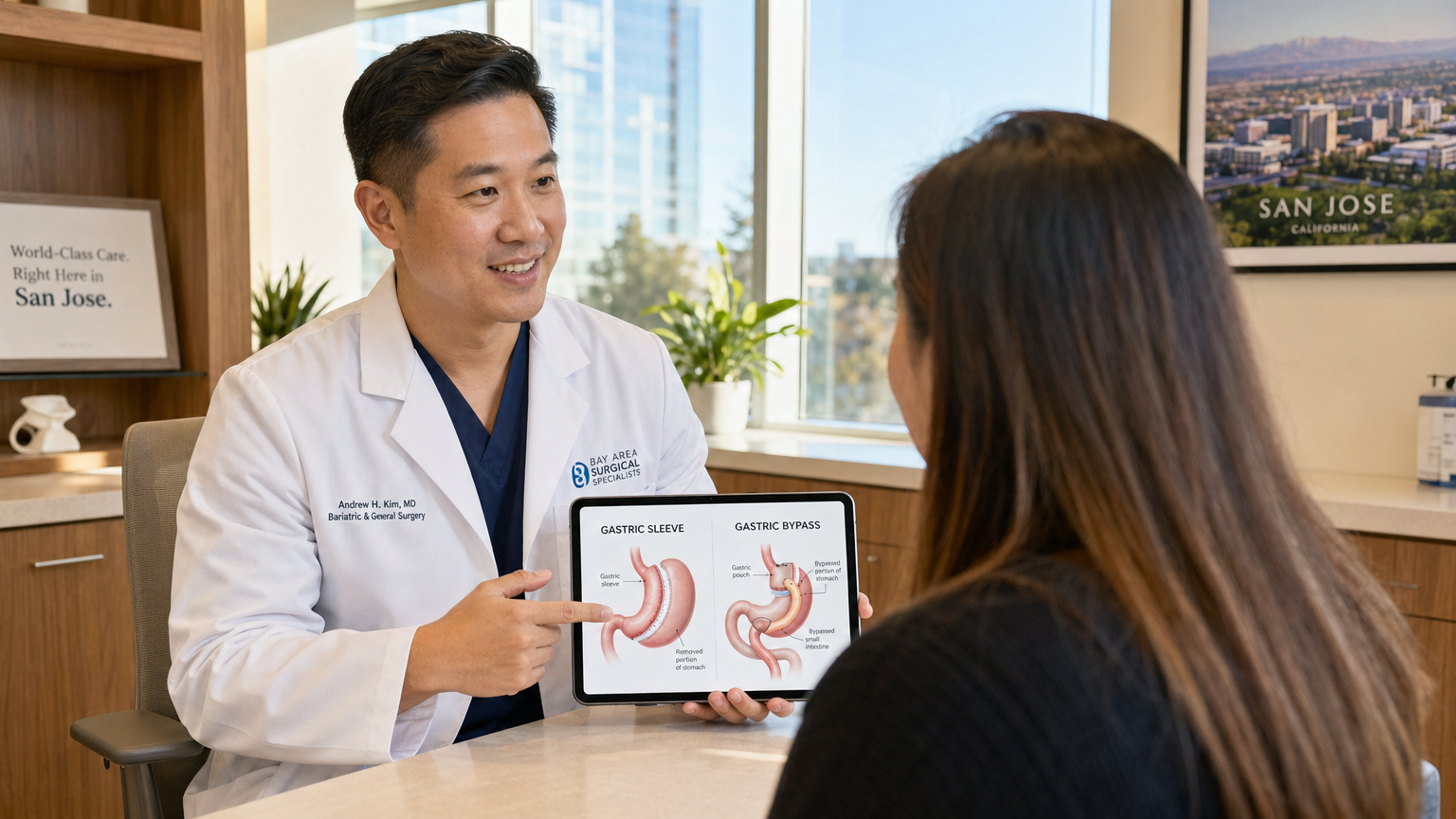
The primary difference between gastric sleeve and gastric bypass lies in how they alter your digestive system. A gastric sleeve removes about 80% of the stomach, restricting food intake and reducing hunger hormones. A gastric bypass creates a small stomach pouch and reroutes the intestines, combining restriction with decreased calorie absorption for more significant weight loss and metabolic changes.
Understanding these fundamental differences is the first step in determining which procedure might be the best fit for your unique anatomical and metabolic needs. Let us delve deeper into the mechanics of each surgery.
The gastric sleeve procedure is currently the most frequently performed bariatric surgery in the United States. During this minimally invasive operation, we remove approximately 80% of the stomach, leaving behind a narrow, banana-shaped "sleeve." This procedure is purely restrictive, meaning it limits the volume of food you can consume at one time. However, it also has a profound metabolic effect. The portion of the stomach that is removed is responsible for producing ghrelin, often referred to as the "hunger hormone." By eliminating this section, patients typically experience a significant reduction in appetite, which is a crucial component of their post-operative success.
Because the intestines are not rerouted during a gastric sleeve, the digestive process remains largely natural. Nutrients are absorbed exactly as they were before the surgery, which simplifies the long-term nutritional requirements compared to other bariatric procedures. This makes the gastric sleeve an excellent option for patients who may be concerned about the complexities of lifelong vitamin supplementation, although basic supplements are still required.
The gastric bypass, often considered the "gold standard" of weight loss surgery, is a more complex procedure that combines restriction with malabsorption. First, we create a small pouch at the top of the stomach, roughly the size of a walnut. This pouch becomes the new stomach, drastically limiting the amount of food you can eat. Next, we divide the small intestine and connect the lower portion directly to the new stomach pouch. The bypassed section of the stomach and the upper portion of the small intestine are then reconnected further down the digestive tract.
This rerouting means that food bypasses a significant portion of the stomach and the first section of the small intestine, where many calories and nutrients are typically absorbed. The combination of eating less and absorbing fewer calories leads to rapid and substantial weight loss. Furthermore, the gastric bypass induces powerful hormonal changes that can rapidly improve or even resolve metabolic conditions such as type 2 diabetes, often before significant weight loss has even occurred.
When comparing gastric sleeve vs gastric bypass, patients naturally want to know which procedure will help them lose the most weight. While individual results vary based on adherence to post-operative lifestyle changes, clinical data provides clear expectations for both surgeries.
Patients who undergo a gastric sleeve typically lose between 60% and 70% of their excess body weight within the first 12 to 18 months. The weight loss is steady and sustainable, provided the patient commits to a healthy diet and regular exercise. The gastric sleeve is highly effective at improving obesity-related conditions, including hypertension, sleep apnea, and joint pain.
The gastric bypass generally yields slightly higher and faster weight loss, with patients typically losing 70% to 80% of their excess body weight in the first year to 18 months. Because of the malabsorptive component and the profound hormonal shifts, the gastric bypass is particularly powerful for patients with severe type 2 diabetes or severe acid reflux (GERD). In fact, for patients suffering from chronic GERD, the gastric bypass is often the preferred procedure, as the gastric sleeve can sometimes exacerbate reflux symptoms.
Both the gastric sleeve and gastric bypass are performed using advanced robotic surgery or laparoscopic techniques at Lifetime Surgical. This minimally invasive approach means smaller incisions, less pain, and a faster return to normal activities compared to traditional open surgery.
The recovery timeline for both procedures is relatively similar. Most patients spend one to two nights in the hospital and can return to desk work within two to three weeks. Full recovery and a return to strenuous activities typically take about four to six weeks. During the initial recovery phase, patients follow a strict, phased diet, progressing from clear liquids to pureed foods, and eventually to solid foods over several weeks.
As with any major surgical procedure, there are risks involved. The gastric sleeve carries a lower risk of surgical complications simply because it is a less complex operation that does not involve rerouting the intestines. Potential risks include staple line leaks, bleeding, and the potential worsening of acid reflux. The gastric bypass, being more complex, carries a slightly higher risk profile, including the possibility of internal hernias, marginal ulcers, and a condition known as "dumping syndrome." Dumping syndrome occurs when high-sugar or high-fat foods move too quickly from the stomach into the small intestine, causing nausea, cramping, and dizziness. While uncomfortable, dumping syndrome often serves as a powerful deterrent against consuming unhealthy foods.
A critical aspect of the gastric sleeve vs gastric bypass comparison is the long-term commitment to nutritional health. Because bariatric surgery alters how you eat and, in the case of bypass, how you absorb nutrients, lifelong supplementation is non-negotiable.
Gastric sleeve patients must take a daily bariatric multivitamin, calcium, and potentially vitamin B12 or iron, depending on their lab results. Because their digestive tract remains intact, the risk of severe nutritional deficiencies is lower than with a bypass, but vigilance is still required.
Gastric bypass patients face a more rigorous nutritional regimen due to the malabsorptive nature of the procedure. They require higher doses of multivitamins, calcium, iron, and vitamin B12. Regular blood work is essential to monitor for deficiencies, which can lead to serious complications such as anemia or osteoporosis if left untreated. Patients must be fully committed to this lifelong regimen to ensure their long-term health and success.
Navigating insurance coverage for bariatric surgery can be complex, but our team at Lifetime Surgical is dedicated to helping patients in San Jose and the Bay Area understand their benefits. Most major insurance providers cover both the gastric sleeve and the gastric bypass, provided the patient meets specific medical criteria. Typically, this includes a Body Mass Index (BMI) of 40 or higher, or a BMI of 35 or higher with at least one obesity-related comorbidity, such as type 2 diabetes, hypertension, or severe sleep apnea.
Insurance companies often require a documented history of medically supervised weight loss attempts, psychological evaluations, and nutritional counseling before approving the surgery. The requirements are generally the same regardless of whether you choose the sleeve or the bypass. Our practice works closely with patients to ensure all prerequisites are met and to streamline the approval process.
| Feature | Gastric Sleeve | Gastric Bypass |
|---|---|---|
| Mechanism | Restrictive (removes 80% of stomach) | Restrictive & Malabsorptive (creates pouch, reroutes intestines) |
| Expected Weight Loss | 60% - 70% of excess weight | 70% - 80% of excess weight |
| Impact on Hunger | Significantly reduces hunger hormone (ghrelin) | Reduces hunger, induces hormonal changes |
| Effect on GERD (Acid Reflux) | May worsen existing GERD | Often resolves or significantly improves GERD |
| Nutritional Risk | Lower risk of deficiencies | Higher risk, requires strict lifelong supplementation |
| Dumping Syndrome Risk | Rare | Common with high-sugar/high-fat foods |
| Surgical Complexity | Lower complexity, shorter operative time | Higher complexity, longer operative time |
Choosing between the gastric sleeve and the gastric bypass is a highly individualized decision that should be made in close consultation with your surgeon. As a general guideline, the gastric sleeve is often an excellent choice for patients who want a less complex surgery, have a lower BMI (though it is effective for high BMIs as well), take multiple medications that need to be fully absorbed, or are concerned about the strict nutritional requirements of a bypass.
Conversely, the gastric bypass is frequently recommended for patients with severe type 2 diabetes, as the metabolic changes can lead to rapid remission. It is also the preferred procedure for patients who suffer from severe acid reflux or GERD, as the bypass anatomy prevents stomach acid from washing up into the esophagus. Additionally, patients with a very high BMI or those who have a significant sweet tooth may benefit more from the bypass, as the risk of dumping syndrome can help curb the intake of sugary foods.
At Lifetime Surgical, we take a comprehensive approach to your care. During your consultation, we will review your medical history, weight loss goals, eating habits, and lifestyle to help you determine the most appropriate path forward. Whether you choose the sleeve or the bypass, our team is committed to supporting you through every step of your transformation.
Yes, a gastric sleeve can be converted to a gastric bypass. This revision surgery is sometimes performed if a patient experiences severe, intractable acid reflux after a sleeve gastrectomy, or if they have not achieved adequate weight loss and require the additional malabsorptive benefits of a bypass.
Many patients experience some degree of loose skin after significant weight loss, regardless of whether they choose the sleeve or the bypass. The amount of loose skin depends on factors such as age, genetics, and the total amount of weight lost. Some patients choose to pursue body contouring surgery after their weight has stabilized for at least a year.
Both procedures are performed under general anesthesia. A gastric sleeve typically takes about 1 to 1.5 hours to complete, while a gastric bypass is a more complex operation that generally takes 2 to 2.5 hours. Because we utilize advanced minimally invasive and robotic techniques, operative times are optimized for patient safety and recovery.
Yes, you will be able to eat normal, solid foods again. However, your portion sizes will be significantly smaller, and you will need to prioritize protein and nutrient-dense foods. The goal of bariatric surgery is not to prevent you from enjoying food, but to help you establish a healthier relationship with eating and achieve long-term wellness.
Ready to take the next step in your weight loss journey? The team at Lifetime Surgical is here to help you achieve lasting health and vitality. Contact us today to schedule a consultation with Dr. Richard Nguyen or Dr. Avery Joseph. Call us at 408-850-0176 or visit our contact page to request an appointment at our San Jose clinic.
Wondering which surgical procedure might be right for your condition? We're here to help you understand your treatment options and develop a personalized surgical plan. Contact our office today to schedule a consultation.
Your path to improved health may be more achievable than you think—with advanced surgical techniques leading to faster recovery, reduced complications, and a significantly enhanced quality of life.